May
Healthcare System Integration Case Study: Improving Diagnostics and Patient Care with APIs

Client Overview
A leading multi-specialty hospital network was struggling with fragmented healthcare IT systems that delayed diagnostics, limited real-time access to patient data, and created inefficiencies across critical care workflows. As patient volumes grew, these disconnected systems began directly impacting care quality, operational speed, and clinical decision-making.
The Challenge
The hospital encountered several critical issues affecting both care delivery and operational performance:
- Disconnected Systems – Patient data was spread across multiple platforms, causing delays and increasing the risk of errors.
- Manual Data Entry – Staff spent significant time transferring data between systems, leading to inefficiencies and inconsistencies.
- Slow Diagnostic Workflows – Radiologists and physicians had to switch between systems, delaying access to complete patient information.
- Limited AI Capabilities – Existing systems were not equipped to support AI-driven diagnostics.
- Compliance Concerns – Maintaining data security and regulatory compliance became complex due to scattered information.
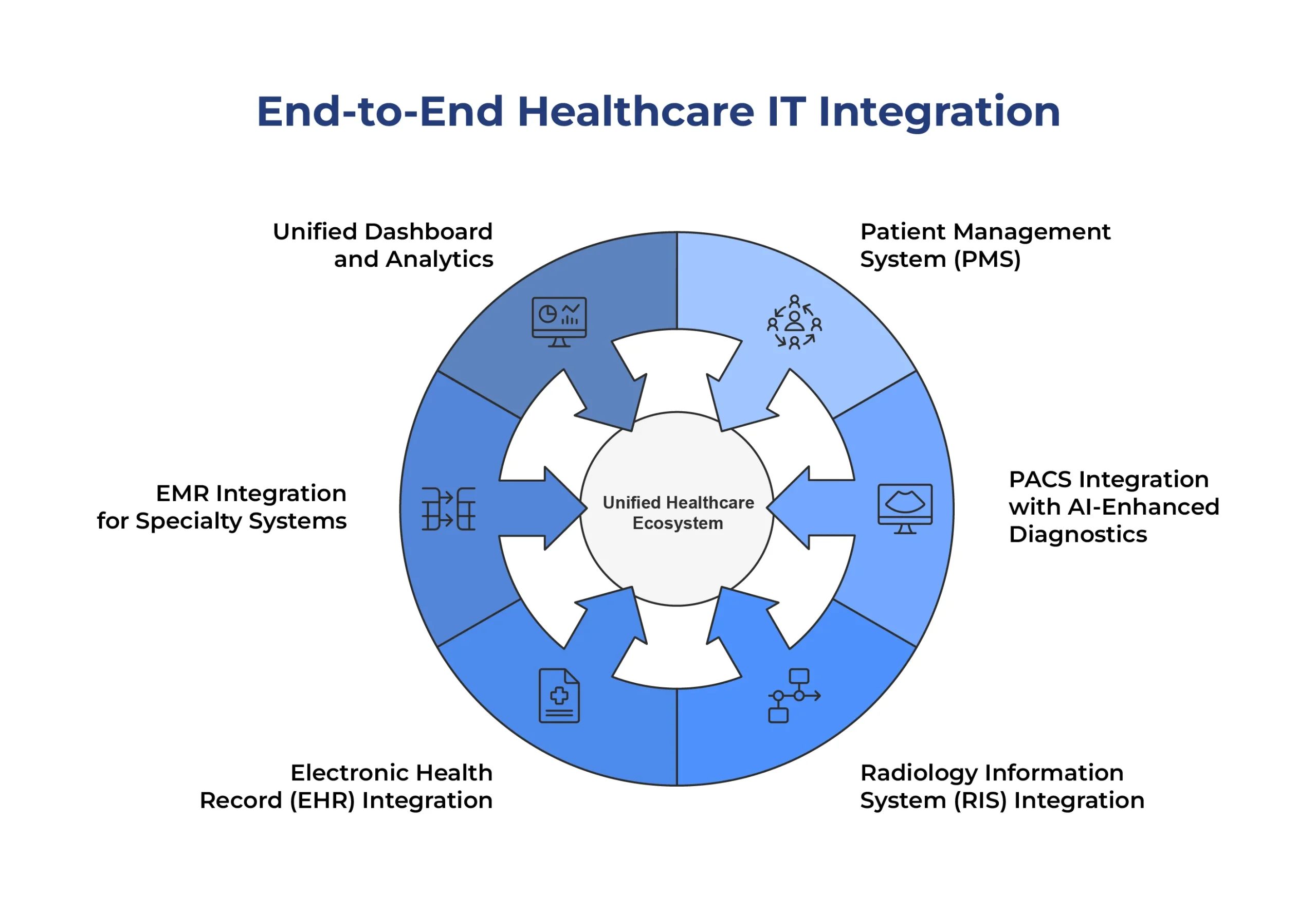
The Solution: End-to-End Healthcare IT Integration
Ficode implemented a comprehensive integration solution, connecting all critical systems into a unified and intelligent healthcare ecosystem.
1. Patient Management System (PMS)
To eliminate data fragmentation and improve coordination, we introduced a centralised Patient Management System that served as a single source of truth across the hospital network.
What We Did:
- Streamlined patient registration, scheduling, and data management into a unified system
- Created a unique patient identifier to eliminate duplicate and inconsistent records
- Designed intuitive dashboards to optimise patient flow and reduce wait times
- Enabled real-time tracking of resources, including bed availability and staff allocation
To eliminate data fragmentation and improve coordination, we introduced a centralised Patient Management System that served as a single source of truth across the hospital network.
Impact:
All departments gained access to accurate, real-time patient information, eliminating data silos and improving coordination.
2. PACS Integration with AI-Enhanced Diagnostics
We integrated PACS across the hospital network and enhanced it with AI to improve diagnostic efficiency.
What We Did:
- Enabled instant access to medical images across systems and locations
- Integrated AI algorithms to detect abnormalities in scans
- Implemented image optimisation and compression techniques
- Built AI-driven priority systems for critical case identification
- Developed tools for automated comparison and measurement analysis
- Enabled secure image sharing for collaboration
Impact:
Radiologists accessed images instantly and benefited from AI-assisted diagnostics, improving accuracy and reducing diagnosis time. Critical cases were prioritised automatically, enhancing patient outcomes.
3. Radiology Information System (RIS) Integration
RIS integration streamlined the radiology workflow from order to reporting.
What We Did:
- Automated exam scheduling through system integration
- Implemented worklist management for radiology teams
- Built structured reporting templates
- Integrated billing for accurate charge capture
Impact:
The radiology department experienced faster workflows, improved coordination, and more efficient reporting processes.
4. Electronic Health Record (EHR) Integration
A unified EHR system was deployed across the hospital.
What We Did:
- Implemented a centralised EHR accessible across departments
- Created specialty-specific templates
- Integrated clinical decision support systems
- Enabled e-prescribing and mobile access for physicians
Impact:
Physicians gained a complete view of patient history in one place, enabling faster and more informed clinical decisions while reducing errors.
5. EMR Integration for Specialty Systems
Specialty departments continued using their own EMR systems while staying connected to the central EHR.
What We Did:
- Integrated specialty EMRs with the central system
- Enabled bi-directional data exchange
- Automated data synchronisation across platforms
- Maintained consistency across all systems
Impact:
Departments retained flexibility while ensuring all patient data remained consistent and accessible across the organisation.
6. Unified Dashboard and Analytics
A central analytics platform was developed to monitor operations and performance.
What We Did:
- Built real-time dashboards for hospital operations
- Created department-specific analytics views
- Implemented predictive analytics for resource planning
- Enabled compliance monitoring and automated reporting
Impact:
Hospital administrators gained real-time insights, enabling better decision-making and improved operational efficiency.
Technical Approach
The solution was built using a scalable and secure architecture:
- HL7 and FHIR standards for interoperability
- API-first design for real-time data exchange
- Cloud infrastructure for scalability and reliability
- Multi-layer security with encryption and access controls
- Microservices architecture for flexibility and easy updates
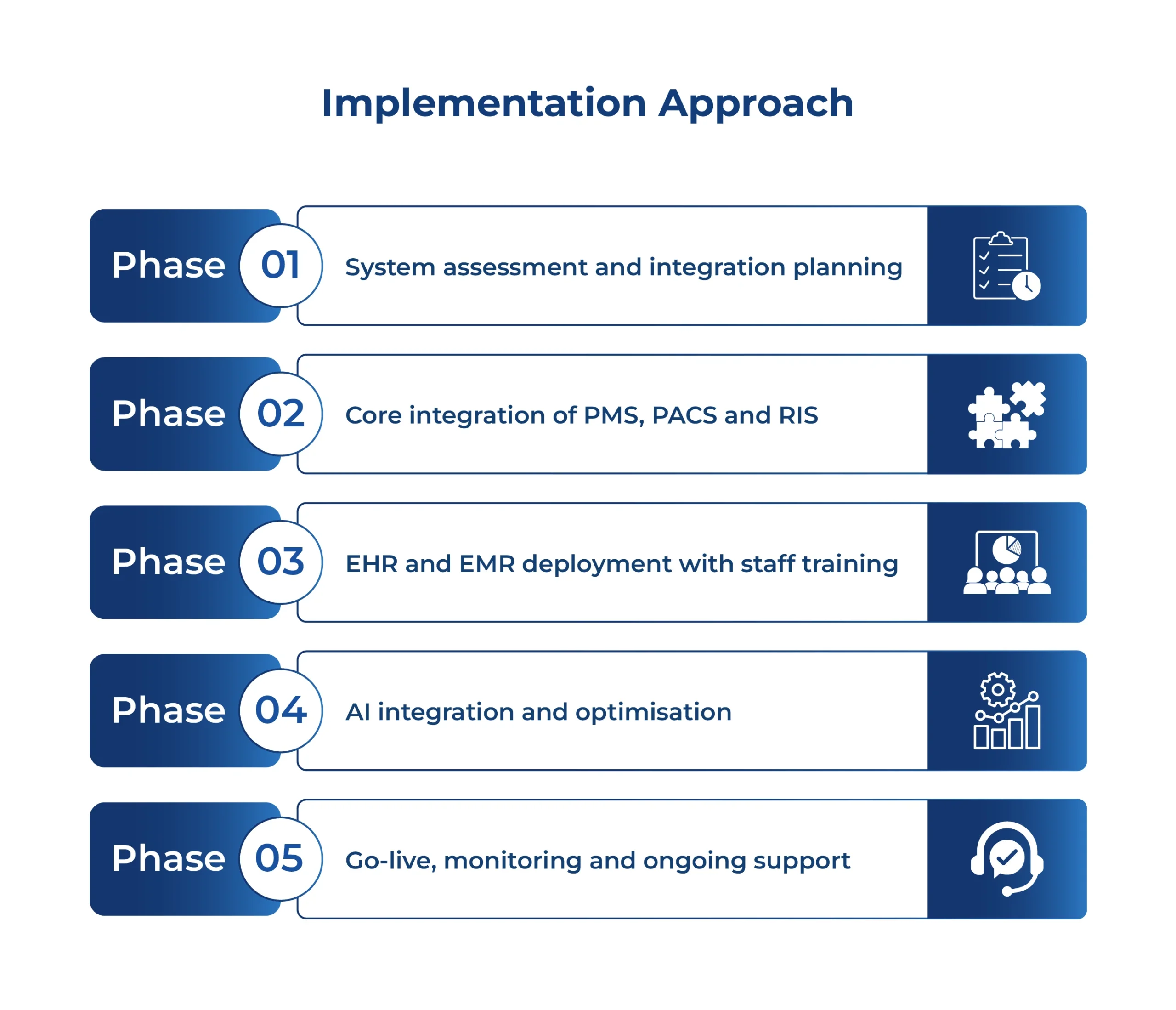
Implementation Approach
The project was delivered through a phased approach:
Key Takeaways
- A holistic integration approach improves overall system efficiency
- Interoperability ensures seamless communication between platforms
- User-centric design aligns technology with real-world workflows
- Phased implementation reduces risk and ensures smooth adoption
- AI enhances clinical capabilities without replacing human expertise
- Strong security measures are essential for healthcare compliance
Business Outcomes
The integration delivered measurable improvements across clinical, operational, and administrative functions:
- Reduced manual data entry, minimising administrative workload and human errors.
- Improved medical image access time across facilities, enabling faster diagnostics and treatment decisions.
- Reduced duplicate patient records, ensuring a more accurate and consistent data environment.
- Improved clinician access to unified records, enhancing care coordination and decision-making.
- Enabled AI-supported triage for critical cases, allowing faster prioritisation and improved patient outcomes.
Conclusion
By integrating PMS, PACS, RIS, EHR, EMR, and analytics systems into a unified ecosystem, Ficode enabled seamless data flow, reduced system fragmentation, and improved diagnostic efficiency across the hospital network. This connected approach also laid the groundwork for AI-driven care, empowering clinicians with faster insights and better coordination.
Planning a healthcare IT integration project? Talk to Ficode about secure, scalable solutions tailored to your workflows.